A wide variety of methods have been used over many decades for treatment of haemorrhoids. Injection sclerotherapy, infrared and laser photocoagulation, cryosurgery, direct application of electrical current, and rubber band ligation all lead to ablation of haemorrhoids unresponsive to conservative management.
Internal haemorrhoids can be graded into 4 stages by using the system of Goligher: |
|
| Grade 1 | haemorrhoids with bleeding |
| Grade 2 | haemorrhoids with bleeding and protrusion, with spontaneous reduction |
| Grade 3 | haemorrhoids with bleeding and protrusion that require manual reduction |
| Grade 4 | haemorrhoids with prolapse that cannot be replaced |
Rubber band ligation has been used to treat internal haemorrhoids since was introduced a ligation device in 1951. Rubber band ligation is now a well established, safe, and effective technique. It has become the mainstay of treatment for bleeding and prolapsing internal haemorrhoids. It has been shown to be substantially better than medication alone in terms of outcome and is not associated with significant morbidity.
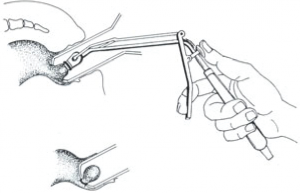
This ligation device is used via an anoscope. Haemorrhoidal tissue is sucked with an applicator and an elastic band is applied. The haemorrhoid and its redundant mucosal tissues become thrombosed and slough, usually within 5 to 7 days. One notable advantage of band ligation is the production of submucosal scarring that prevents subsequent development of new haemorrhoidal tissue.
Rubber band ligation technically is simple and can be used in the outpatient setting without local anaesthesia. The success rate lays between 69% and 97%, depending on the degree of internal haemorrhoids, the ligation technique, and the duration of follow-up.
Conventional band ligation is performed with a rigid anoscopic device, which has videoscopic capability to document treatments. Many studies have assessed the safety and efficacy of rubber band ligation by using a video-endoscopy system for treatment of patients with symptoms caused by internal haemorrhoids.
 The treatment is reserved for patients with grade 2 to 4 internal haemorrhoids, presenting with rectal bleeding and/or prolapse unresponsive to medication. Usually two or more sessions of endoscopic haemorrhoidal ligation are necessary.
The treatment is reserved for patients with grade 2 to 4 internal haemorrhoids, presenting with rectal bleeding and/or prolapse unresponsive to medication. Usually two or more sessions of endoscopic haemorrhoidal ligation are necessary.
Rectal bleeding is usually the main symptom. Other complaints are bleeding combined with rectal prolapse; intermittent dripping of blood from the anal area; and the notice of blood occasionally on toilet tissue. Rectal prolapse is the major complaint with intermittent mild rectal bleeding.
 All patients should undergo flexible sigmoidoscopy or colonoscopy to exclude other causes of bleeding per rectum.
All patients should undergo flexible sigmoidoscopy or colonoscopy to exclude other causes of bleeding per rectum.
All patients must be educated about the procedure and give informed consent prior to treatment.
Patients do not need to discontinue the use of aspirin or other non-steroid anti-inflammatory medication before the procedures. After the endoscopic examination, patients are treated if grade 2 or larger internal haemorrhoids were present. The dentate line in the anal canal is identified, and ligation under suction is performed 2 to 5 mm above the dentate line. All ligations were performed in the outpatient setting. Safety data are recorded; all events are documented in the report given to the patient.
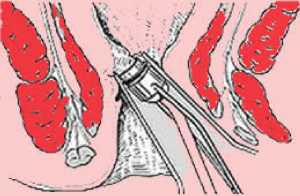 The ligation procedure is completed in less than 10 minutes in most cases.
The ligation procedure is completed in less than 10 minutes in most cases.
A mean of 3 rubber bands are placed per session.
A reduction of at least one grade is achieved in most cases. Many patients will have the urge to go to the toilet and some patients may have mild anal pain which can relieved by orally administered diclofenac. Mild bleeding may occur which rarely needs injection of a dilute solution of epinephrine (1:100,000).
Patients are seen 4 to 6 weeks later and then at 2 months interval if necessary. If residual haemorrhoids are noted or symptoms persisted, further treatments were conducted monthly. The end point of treatment is to achieve grade 1 haemorrhoids.
Serious complications, such as life-threatening massive bleeding and sepsis, are extremely rare, but cannot be fully discounted. Videoendoscopic anoscopy and a single-handed ligator compared favourably with traditional haemorrhoid banding by anoscopy. Video endoscopic techniques are preferred in the office setting.
Endoscopic haemorrhoid ligation is an important adjunct in the treatment of patients with symptomatic internal haemorrhoids. Haemorrhoidal ligation is simple, safe, and effective. Multiple bands can be applied in one session, and the treatment repeated to completely eradicate the internal haemorrhoids. The treatment success rate is high, and the long-term recurrence rate is low.